Chiropractic Thermography
Thermal Imaging in Chiropractic
Thermography has been a part of chiropractic analysis since the early days of the profession, particularly through the work of B.J. Palmer. The dual-point approach, which compares temperature differences between bilateral points along the spine, has deep historical roots and was one of the earliest attempts to introduce objective measurement into chiropractic practice. However, there are inherent limitations in relying on only two points of comparison. The human body is not perfectly symmetrical. Variations such as scars, skin folds, hairlines, minor skin conditions, and postural differences all influence surface temperature. These factors introduce variability that can affect readings independent of underlying physiology, making strict bilateral comparison inherently unreliable. Additionally, as a thermal device is scanned across the body, it captures temperature at a single point in time and space. While infrared measurement itself is highly accurate, the clinical value of an isolated point is limited. Without context, a single measurement does not reflect the broader thermal landscape or the physiologic patterns that govern temperature distribution. For these reasons, dual-point analysis represents an early but incomplete method of thermographic assessment. Modern approaches favor full-field imaging and pattern evaluation across regions, allowing for a more accurate and clinically meaningful interpretation of physiologic function.
Tech Spotlight: A Clearer, Smarter View
Digital thermal imaging changes the game. A modern 640×480 thermal camera captures up to 307,000 individual temperature points — providing a much more complete and precise image of the body’s thermal profile. Even better, prices for these advanced cameras have dropped significantly in recent years — now often costing less than traditional dual point equipment.
Philosophy Aligns with Physiology
History of Thermography in Chiropractic
Thermography has held a distinct and enduring role within chiropractic, rooted in the profession’s long-standing interest in functional assessment of the nervous system. From its earliest days, chiropractic has sought objective methods to evaluate physiologic change—particularly as it relates to autonomic regulation and spinal function.
Before modern infrared imaging, chiropractors utilized early temperature-measuring instruments such as the neurocalometer and later the nervoscope. These devices focused on detecting segmental temperature differences along the spine, based on the premise that altered nerve function could influence cutaneous blood flow and, therefore, skin temperature. While limited to single-point or dual-point measurements, these instruments represented one of the first attempts in healthcare to quantify physiologic change in a reproducible way.
As infrared technology advanced in the mid-20th century, thermography expanded beyond point measurement into full-field imaging. This transition marked a significant shift. Instead of evaluating isolated spinal segments, practitioners could now observe broader thermal distributions across the body, providing a more comprehensive view of autonomic and vascular activity.
Within chiropractic, thermography became particularly relevant in the assessment of neuromuscular and autonomic function. The relationship between spinal nerve involvement and peripheral temperature changes supported its use as an adjunctive tool in evaluating nerve root dysfunction, peripheral nerve injury, and sympathetic regulation.
Over time, continued improvements in camera technology—particularly the development of high-resolution, radiometric systems—further refined the clinical application of thermography. These advancements allowed for precise temperature measurement across the entire image, reducing reliance on isolated readings and improving reproducibility.
Today, chiropractic thermography is best understood as a physiologic assessment tool. It does not visualize structure or diagnose pathology directly, but instead reflects changes in cutaneous blood flow under autonomic control. This aligns closely with chiropractic’s emphasis on function over structure and reinforces its role as a complementary tool in clinical evaluation.
The progression from early spinal temperature instruments to modern radiometric imaging represents not a departure from chiropractic principles, but an evolution toward greater accuracy, consistency, and scientific grounding in the assessment of human physiology.
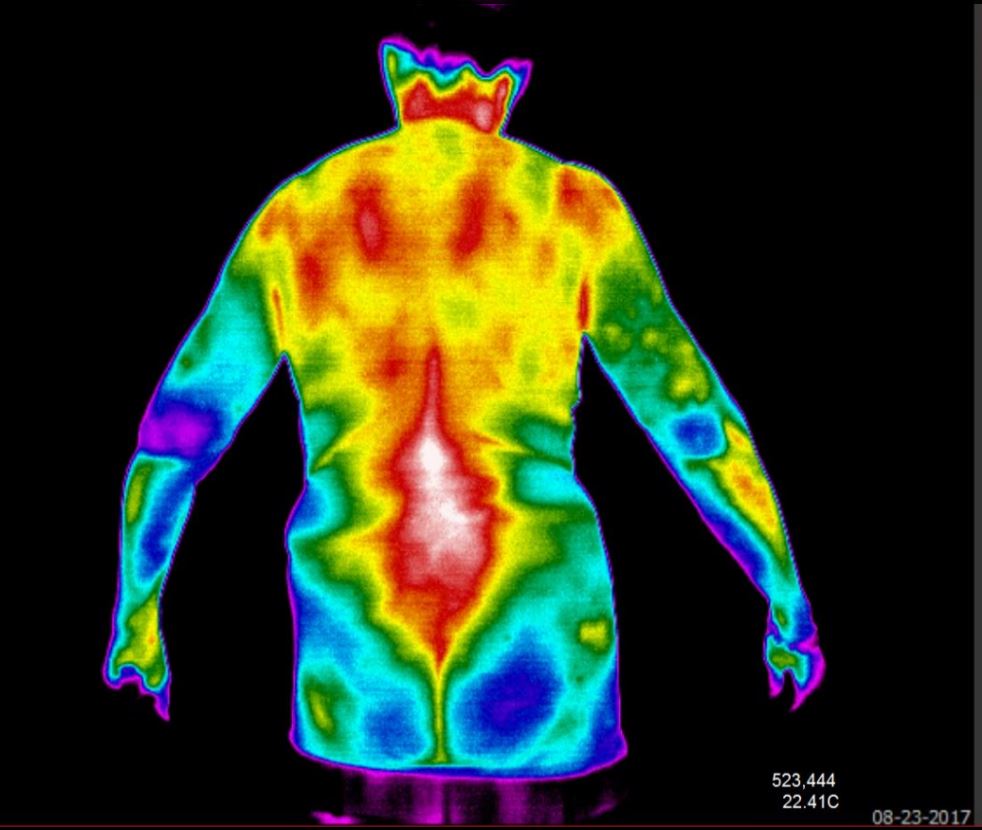
The Evolution of Pattern Analysis in Chiropractic Thermography
Thermography has played a unique role in chiropractic for decades, particularly in the evaluation of spinal function through temperature patterns. Early systems focused on identifying repeatable thermal patterns along the spine, with the interpretation that a patient who remained “in pattern” reflected an ongoing state of dysfunction.
As technology and understanding have advanced, so has the interpretation of these patterns.
Modern thermography has shifted from isolated measurements and pattern-based assumptions toward a broader physiologic perspective. It is now well understood that thermal patterns are often highly reproducible under controlled conditions. Rather than representing abnormality, these patterns frequently reflect an individual’s baseline autonomic and vascular regulation—essentially a thermographic “fingerprint.”
This evolution has led to a more refined clinical approach. Instead of focusing on whether a pattern is present or “broken,” emphasis is placed on meaningful change over time. True physiologic alterations are distinguished from transient surface effects, such as those caused by contact, pressure, or environmental influences.
This progression—from early pattern interpretation to modern radiometric analysis—represents a maturation of chiropractic thermography. It reflects a move toward greater accuracy, reproducibility, and alignment with known physiologic principles, while still honoring the foundational role thermography has played in chiropractic assessment.
Bald Men are Never Subluxated
Hair Artifact in Upper Cervical Dual-Point Analysis
In upper cervical dual-point thermographic analysis, a temperature difference of approximately 1°C at the atlas is commonly observed. Historically, this finding has often been interpreted as clinically significant. However, a critical confounding factor must be considered: hair.
Hair has a lower emissivity and typically registers cooler than exposed skin on infrared imaging. When a measurement point overlies the hairline on one side and exposed skin on the other, an artificial temperature differential may be introduced. This can create the appearance of a thermal asymmetry where none physiologically exists.
A simple experimental demonstration highlights this effect. When dual-point measurements are performed on an individual with hair present at the atlas region, a temperature difference may be observed. If the same individual is re-evaluated after shaving the hair in that region, the previously noted asymmetry often resolves.
This observation is further supported by the relative absence of consistent atlas-level thermal asymmetry in individuals without hair in that region.
Clinical Implication
These findings suggest that at least some historically reported upper cervical thermal “breaks” may represent measurement artifact rather than true physiologic change. This reinforces a broader principle in thermographic interpretation:
-
Surface conditions (hair, skin texture, moisture) directly affect infrared readings
-
Small, localized temperature differences must be interpreted within full image context
-
Single-point or dual-point measurements are particularly vulnerable to artifact
Chirotherm analysis procedures are designed with these limitations in mind. Rather than relying on isolated point measurements, they incorporate full-field radiometric imaging, standardized patient preparation, and strict protocol controls to minimize surface-related artifacts such as hair interference. This allows for a more reliable assessment of physiologic thermal patterns rather than misleading focal discrepancies.
Failure to account for these factors can lead to overinterpretation and erroneous clinical conclusions.
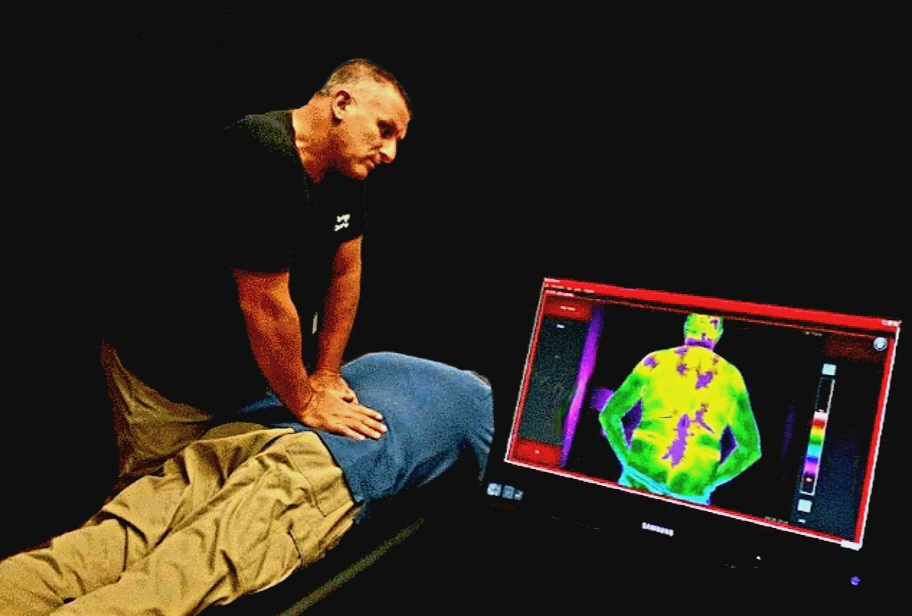
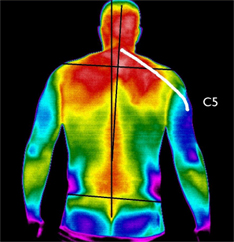
Monitoring Progress with Objective Thermal Imaging
Clinical Value of Thermography in Chiropractic Practice
Thermography provides objective, reproducible measurements that can be tracked over the course of care. When performed under controlled conditions, these measurements allow for meaningful comparison over time, offering a visual and quantitative record of physiologic change.
This has practical value for both the clinician and the patient. Patients are able to visualize their condition directly on the screen, reinforcing clinical findings and improving understanding of their care. As treatment progresses, changes in thermal patterns can be observed and documented, providing an additional layer of outcome assessment.
For the chiropractor, thermography serves as a useful adjunct in evaluating neuromuscular and autonomic function. Areas of decreased temperature may be associated with reduced blood flow or sympathetic-mediated vasoconstriction, often seen in nerve-related dysfunction. Conversely, areas of increased temperature may reflect inflammation or increased metabolic activity.
Used appropriately, thermography supports a more objective, physiologic approach to chiropractic care and represents a step toward integrating modern measurement technologies into clinical practice.
